You know that moment when a patient walks into your clinic complaining of palpitations, but their resting ECG looks perfectly normal? It’s frustrating, right? You know something’s happening, but you just can’t catch it in that 10-second window. That’s exactly where ECG Holter monitors become your best diagnostic ally.
I’ve watched this technology evolve from bulky, uncomfortable devices that patients dreaded wearing to sleek, barely-there patches that seamlessly integrate into daily life. And honestly? The advances we’re seeing in 2026 are nothing short of remarkable.
Let me take you through everything you need to know about Holter monitoring—from the basics to the cutting-edge options that are changing cardiac care in Sri Lanka and beyond.
What Exactly Is an ECG Holter Monitor?
Here’s the simple truth: an ECG Holter monitor is a small, wearable device that continuously records your patient’s heart rhythm for 24-48 hours (or longer). Think of it as your eyes on the heart when you can’t be there—capturing every beat, every irregularity, every tell-tale sign that might explain those mysterious symptoms.
Unlike that quick ECG snapshot you take in the office, a Holter monitor is the marathon runner of cardiac diagnostics. It’s there when your patient climbs stairs, feels stressed at work, or experiences that 3 AM episode they can’t quite describe. It’s continuous, uninterrupted cardiac surveillance.
Insert image of modern Holter monitor attached to patient’s chest here
The beauty of Holter monitoring lies in its simplicity and effectiveness. While you’re catching maybe 10 seconds of cardiac activity with a standard ECG, the Holter is recording 100,000+ heartbeats over a 24-hour period. That’s a lot of data—and a lot of opportunities to catch intermittent arrhythmias that love playing hide-and-seek.
How Long Should Your Patient Wear a Holter Monitor?
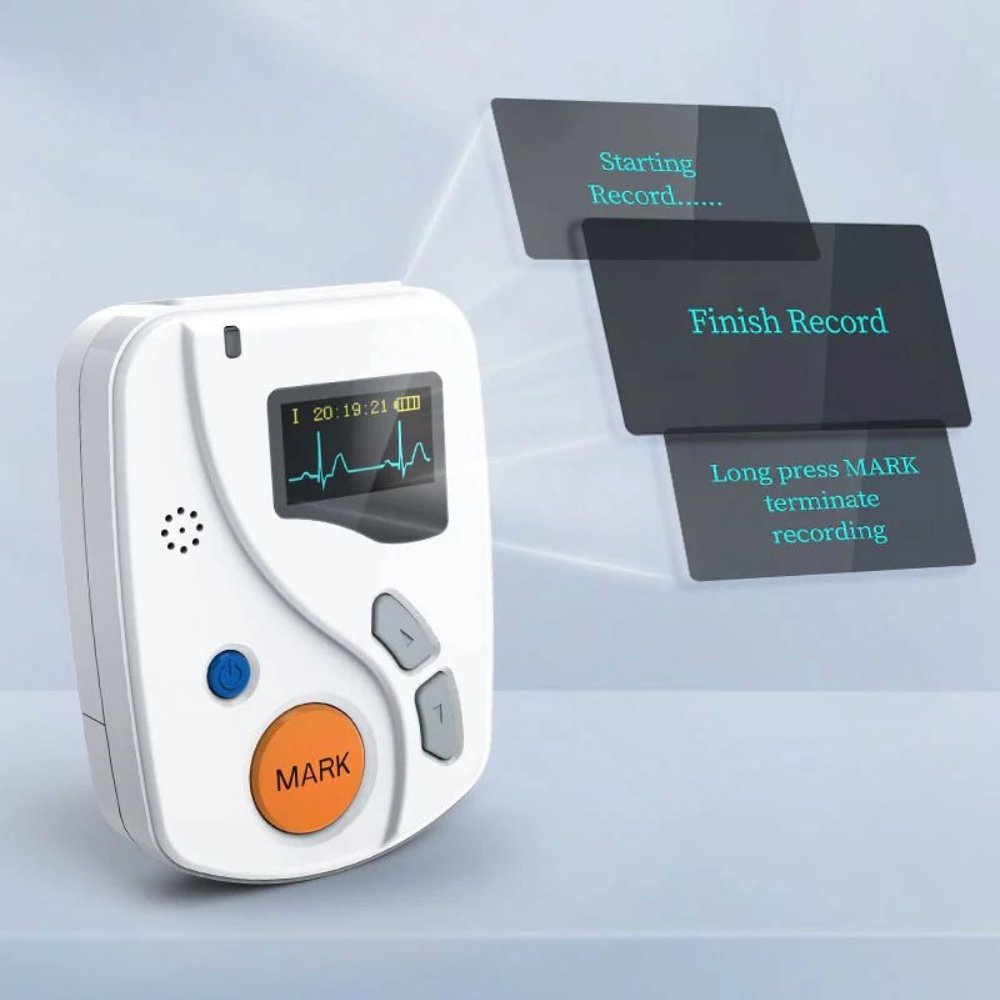
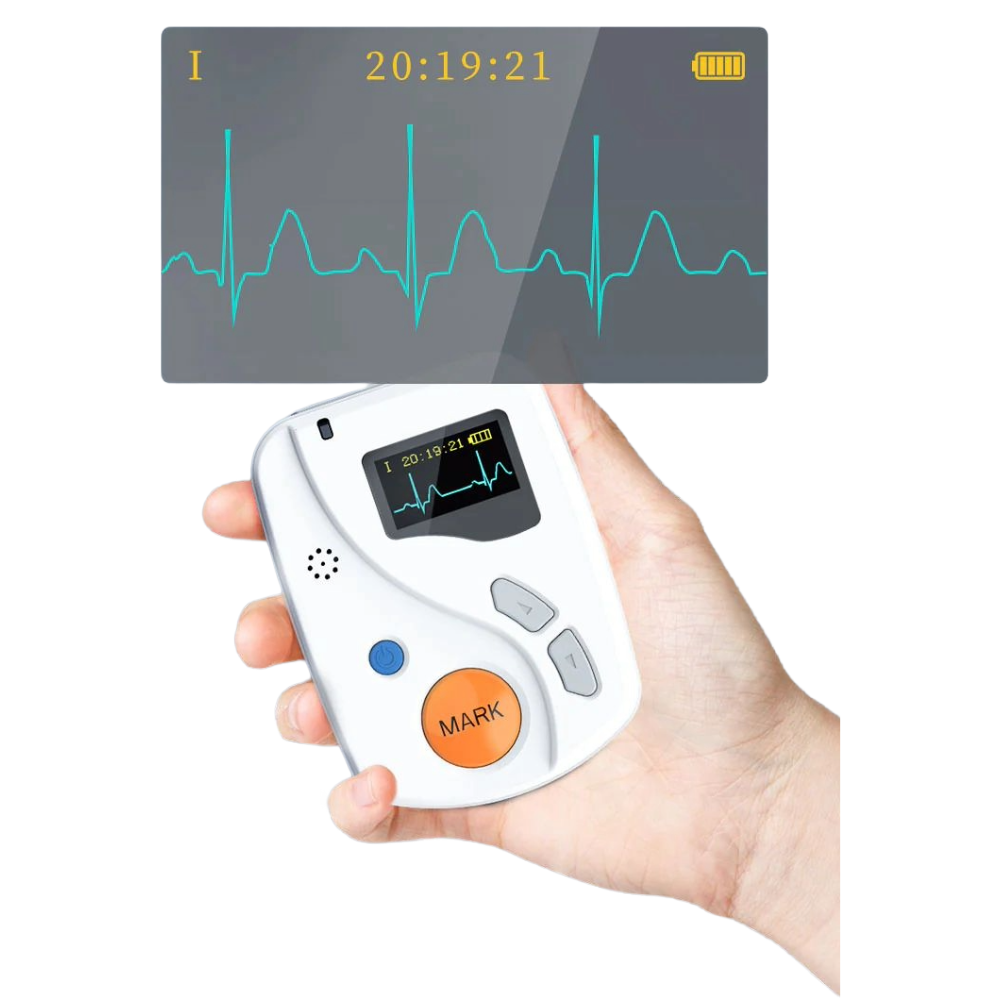
The standard answer? Typically 24-48 hours. But here’s where it gets interesting—and where your clinical judgment really matters.
For straightforward cases where you suspect relatively frequent arrhythmias, 24 hours usually does the trick. I’ve found this duration captures most daily activity patterns: morning routines, work stress, exercise, meals, and sleep cycles. It’s the goldilocks zone—long enough to be useful, short enough to maintain patient compliance.
However, if you’re dealing with less frequent symptoms or if that first 24-hour recording comes back frustratingly normal despite persistent patient complaints, extended monitoring up to 7-14 days becomes invaluable. Think about it: some arrhythmias are like rare birds—you need patience and extended observation to spot them.
The newer wireless models make extended wear much more tolerable. Patients aren’t tethered to a brick-sized recorder anymore. They’re wearing something closer to a large bandage, which dramatically improves compliance and quality of life during monitoring.
The Shower Question: Can Patients Get Wet?
I’ll be straight with you: No, most Holter monitors are not waterproof. And yes, this is probably the question your patients will ask first, right after “Will it hurt?”
Here’s what I tell patients: shower before we apply the monitor, and plan on skipping baths and showers until it comes off. It’s not ideal, but it’s temporary. For those concerned about hygiene, a gentle sponge bath avoiding the chest area usually works fine.
The electrodes need consistent, dry contact with the skin to maintain signal quality. Water exposure can loosen adhesion, cause artifacts in the recording, or worst case, damage the device. And trust me, a recording ruined by water exposure means starting over—something neither you nor your patient wants.
Pro tip: Some of the newer patch-based monitors like the Zio Patch by iRhythm offer improved water resistance for quick showers, but always check manufacturer specifications. When in doubt, keep it dry.
ECG vs. Holter Monitor: What’s the Real Difference?
Let me paint you a picture. A standard ECG is like taking a single photograph of a sunset. Beautiful, informative, captures a moment—but tells you nothing about how that sunset developed or what happened after you clicked the shutter.
A Holter monitor? That’s your time-lapse video of the entire day, from dawn to dusk and through the night.
Key differences:
- Duration: ECG captures 10 seconds; Holter records 24-48+ hours continuously
- Scope: ECG shows current rhythm; Holter reveals rhythm patterns, variability, and intermittent events
- Context: ECG is clinic-based and anxiety-inducing for some patients; Holter captures real-world activity
- Diagnostic yield: ECG might miss paroxysmal arrhythmias; Holter significantly increases detection rates
Here’s what really matters for your practice: studies show that Holter monitoring increases arrhythmia detection by up to 50% compared to standard ECG alone for patients with intermittent symptoms. That’s a massive diagnostic improvement.
Insert comparison table image here
Is Holter Monitoring Painful? Let’s Talk Comfort
Absolutely not painful. But let me be completely honest with you—and with your patients—it’s not exactly “comfortable” either, especially by day two.
The device itself causes zero pain. There are no needles, no invasive procedures, no discomfort from the monitoring process. What patients do experience is:
- Mild skin irritation from electrode adhesive (quite common, especially in humid Sri Lankan climate)
- Itching around electrode sites
- Slight discomfort from sleeping with wires or the recorder unit
- Self-consciousness about the visible leads and device
I always warn patients that by hour 36, they’ll be counting down to removal. The adhesive gets sticky, the skin gets irritated, and everyone’s just done with it. But that mild discomfort is temporary and vastly outweighed by the diagnostic value.
For patients with sensitive skin, applying a barrier wipe before electrode placement can reduce irritation. It’s a small step that significantly improves patient experience.
Exercise and Activity: Should Patients Maintain Normal Routines?
Yes, absolutely—and this is crucial for diagnostic accuracy. In fact, I encourage patients to maintain their usual activity levels, including light to moderate exercise.
Here’s why: many arrhythmias are exercise-induced or stress-related. If your patient sits perfectly still for 24 hours trying to “protect” the monitor, you’ll miss exactly the data you need. You want to capture their heart’s response to daily life stressors—climbing stairs, carrying groceries, dealing with work deadlines, even having an argument with their teenager.
That said, there are sensible limits:
- Avoid: swimming, contact sports, activities causing excessive sweating that might loosen electrodes
- Encourage: walking, light housework, normal work activities, using stairs
- Perfect: keeping a detailed symptom diary noting activities and any palpitations or chest discomfort
The diary is gold. When you’re reviewing that Holter data and spot a run of ventricular ectopy at 2:47 PM, being able to correlate it with “climbing three flights of stairs” or “heated phone call” provides invaluable clinical context.
How Holter Results Get Analyzed: Behind the Scenes
This is where technology meets clinical expertise—and it’s honestly one of the most fascinating parts of modern cardiology.
The process:
Once your patient returns the device, the data gets downloaded to specialized Holter analysis software. Modern systems use sophisticated algorithms that can:
- Automatically detect and classify arrhythmias (atrial fibrillation, ventricular tachycardia, premature beats)
- Calculate heart rate variability
- Identify ST-segment changes suggesting ischemia
- Flag abnormal pauses or bradycardia
- Generate detailed reports with thousands of data points compressed into clinically meaningful summaries
But here’s the critical part: automated analysis is never the final word. You or another cardiologist must review the raw data strips, verify automated classifications, and correlate findings with the patient’s symptom diary. Software can flag what looks like ventricular tachycardia, but you need to rule out artifacts from brushing teeth or other muscle movements.
The best Holter reports I’ve seen present data in tiers:
- Executive summary: key findings, burden of arrhythmias, correlation with symptoms
- Detailed rhythm analysis: hourly trends, rate histograms, sample strips of significant events
- Raw data availability: for deep dives when needed
Insert image showing sample Holter report interface here
When Holter Comes Back Normal: Now What?
It happens. You send a patient home with a Holter, they experience their typical symptoms, and the recording shows… perfectly normal sinus rhythm. Frustrating? Absolutely. But it’s not the end of the road.
This scenario suggests one of three possibilities:
- Symptoms are genuinely non-cardiac (anxiety, musculoskeletal, GI)
- Arrhythmia burden is extremely low and you simply didn’t capture an event
- You need longer or different monitoring strategy
This is where event monitors or mobile cardiac telemetry become your next tool. Unlike continuous recording, event monitors capture data only when patients activate them during symptoms, or when the device automatically detects significant arrhythmias. For infrequent symptoms occurring once weekly or less, event monitors with 30-day wear periods make more sense than Holter.
I’ve had patients where it took a 30-day event monitor to finally catch that elusive paroxysmal atrial fibrillation that was hiding from every 24-hour Holter. Persistence pays off.
Can a Holter Monitor Detect Anxiety?
Short answer: No. A Holter records heart rhythm—the electrical patterns and rate variations—but it cannot diagnose psychological or psychiatric conditions.
However—and this is important—Holter monitoring can help differentiate cardiac arrhythmias from anxiety-related symptoms. When patients report palpitations, dizziness, or chest discomfort, Holter data showing completely normal rhythm during symptomatic episodes can provide powerful reassurance that the heart itself is healthy.
Sinus tachycardia during episodes of reported palpitations, coupled with normal underlying rhythm and no arrhythmias, strongly suggests an anxiety component. This information allows you to confidently shift focus toward appropriate anxiety management rather than continuing an endless cardiac workup.
It’s not that anxiety is “less real”—it’s that knowing the heart is structurally and electrically sound changes your therapeutic approach entirely.
Electrode Placement: Getting It Right
Standard placement involves 3-7 electrodes on the chest wall, typically in modified precordial positions. The exact configuration depends on whether you’re doing 3-channel, 5-channel, or 12-lead Holter recording.
Here’s what matters clinically:
Skin preparation is everything. Shave chest hair if present (yes, have this conversation beforehand), clean with alcohol, let dry completely, and then apply electrodes. Poor adhesion from oily skin or inadequate prep is the number one cause of recording failure.
For patients with very hairy chests, I explain upfront that shaving a few small areas is necessary. Most accept this when they understand it’s essential for accurate recording. Those who refuse need to understand they’re risking poor data quality and possible need to repeat the test.
The electrodes stay put for the entire monitoring period—no adjustments, no peeking underneath, no “checking if it’s still there.” Any disruption compromises signal quality.
Insert diagram showing proper electrode placement positions here

When Do Results Come Back?
Typically within 1-2 weeks after device return. This timeframe accounts for:
- Data download and initial automated analysis (minutes to hours)
- Cardiologist review and interpretation (variable depending on workload and complexity)
- Report generation and communication to referring physician
In urgent situations—suspected life-threatening arrhythmias, severe symptoms—analysis can be expedited to within 24-48 hours. Most centers prioritize based on clinical urgency indicated on the requisition.
For routine screening or follow-up monitoring, the 1-2 week timeline is standard. Set patient expectations accordingly so they’re not calling your office daily asking for results.
Sleeping With a Holter: Why It’s Non-Negotiable
Yes, patients must sleep with the device on. This isn’t optional, and here’s why it matters tremendously.
Many significant arrhythmias occur during sleep:
- Sleep apnea-related bradycardia and pauses
- Nocturnal atrial fibrillation (surprisingly common)
- REM-related arrhythmias
- Vagally-mediated heart blocks
I’ve diagnosed countless cases of significant nocturnal arrhythmias that were completely asymptomatic—patients had zero awareness anything was happening while they slept. Missing the nighttime data means missing potentially critical findings.
For patients worried about comfort, suggest sleeping on their back or the side opposite the recorder. Most adapt within one night. Yes, it’s annoying. Yes, it’s necessary.
Top ECG Holter Monitors for 2026: What’s Worth Considering
Let me walk you through the devices that are genuinely making a difference in clinical practice this year. I’ve had hands-on experience with several of these, and I’ve heard consistent feedback from colleagues across Sri Lanka and internationally.
Premium Tier: Clinical Excellence
1. Bittium Faros 180
This Finnish-engineered device has become my go-to for extended monitoring. Lightweight (under 15 grams), reliable 7-14 day battery life, and Bluetooth connectivity for real-time data transmission. The form factor is genuinely impressive—patients often forget they’re wearing it by day three.
Price point: approximately $600-800 per unit
Best for: Extended arrhythmia detection, AFib screening programs, research applications
2. Philips BioTel Heart Monitor
The 30-day wireless patch format represents where the industry is heading. App integration allows patients to log symptoms directly on their smartphone, and the telehealth integration has streamlined my remote monitoring workflow considerably.
Price point: typically offered through monitoring services rather than direct purchase
Best for: Practices with established telehealth infrastructure, tech-comfortable patients
3. Zio Patch by iRhythm
The disposable adhesive format eliminates patient concerns about returning equipment. No wires, no separate recorder unit—just apply and forget for up to 14 days. The AI-enhanced analysis catches subtle findings I’ve occasionally missed on manual review.
Price point: $200-400 per patch (disposable)
Best for: High patient volume practices, patients anxious about equipment responsibility
Insert image showing size comparison of modern patch monitors here
Mid-Tier: Excellent Value
4. GE SEER 1000
A clinic workhorse. Not fancy, not wireless, but absolutely reliable. Single-lead with event button functionality allows patients to mark symptomatic episodes—helpful for correlation during analysis.
Price point: $300-450
Best for: Budget-conscious practices wanting proven reliability
5. Schiller Medilog AR4
High-resolution 7-day recording with impressive AI analysis software. The European engineering shows—robust build quality and intuitive software interface. Popular among academic centers for research-grade data.
Price point: $700-900
Best for: Centers prioritizing detailed analysis and research applications
6. CardioMem CM3000
Three-channel portable that hits the sweet spot of affordability and functionality. It’s not breaking any technological boundaries, but it reliably captures the data you need for routine clinical use.
Price point: $250-400
Best for: Small clinics, rural healthcare settings, cost-sensitive markets
Budget-Friendly Options

Hugely popular in India and increasingly seen in Sri Lankan clinics. Basic 24-hour monitoring with USB download. No frills, but it works. Software could be more intuitive, but at this price point, it’s hard to complain.
Price point: $150-250
Best for: High-volume screening, budget-constrained settings
8. BPL Holter 601
Another Indian-market favorite offering 24/48-hour recording. Cost-effective for practices just starting Holter services or needing multiple units for high patient volume.
Price point: $180-300
Best for: Indian subcontinent practices, price-sensitive markets
Specialized Applications
9. Preventice BodyGuardian Mini
Miniaturized specifically with athletes in mind, with waterproof options for active patients. If you’re working with sports cardiology or younger, active populations, this addresses the lifestyle compatibility issue better than traditional models.
10. Mortara Ambulatory
The 12-lead capability sets this apart. When you need true 12-lead ECG data over 24 hours—thinking about ischemia detection or detailed repolarization analysis—this hospital-grade device delivers.
Holter Monitor vs. Event Monitor: Choosing Wisely
This decision matters more than many clinicians realize. Choose Holter when:
- Symptoms occur daily or near-daily
- You need comprehensive rhythm assessment over a defined period
- Screening for paroxysmal AFib in high-risk patients
- Post-ablation monitoring
- Evaluating medication efficacy
Choose event monitors when:
- Symptoms are infrequent (less than 3-4 times weekly)
- Patient needs to trigger recording during symptoms
- Extended 30-day monitoring makes more sense
- Cost constraints favor longer monitoring with episodic recording
I’ve made the mistake of sending patients home with 24-hour Holters when their symptoms occurred weekly—predictably, we caught nothing and had to repeat with proper event monitoring. Learn from my errors: match the device to symptom frequency.
Insert comparison table: Holter vs. Event Monitor specifications here
Buying Considerations: What Matters Beyond Price
When you’re ready to invest in Holter monitoring for your practice, price is obviously important—but it shouldn’t be your only consideration.
Critical factors:
Software quality: You’ll spend hours with this interface. Clunky, unintuitive software turns analysis into a frustrating chore. Demo the software thoroughly before purchasing.
Technical support: When (not if) you encounter technical issues, responsive support makes the difference between minor inconvenience and lost patient data. Check support availability in Sri Lanka specifically.
Battery life reliability: Nothing worse than incomplete recordings due to battery failure. Look for devices with proven track records and battery life exceeding stated monitoring duration by 20%+.
Durability: These devices get handled roughly despite instructions otherwise. Robust construction pays off over years of clinical use.
FDA/CE approval: For clinical use, ensure proper regulatory approval. This matters for liability and insurance reimbursement.
Electrode quality: Cheap electrodes false-save money but cause endless artifacts and poor adhesion. Factor quality electrodes into your total cost calculation.
Interpreting Holter Results: What You’re Actually Looking For
Let’s talk about the clinical meat of Holter monitoring—what findings actually matter and how to communicate them effectively.
Key diagnostic targets:
Atrial fibrillation burden: Not just presence/absence, but percentage of recording time spent in AFib. A 10-minute AFib episode has very different implications than 12 hours of persistent AFib.
Ventricular ectopy: Frequency, patterns (bigeminy, couplets, salvos), and QRS morphology. That isolated PVC? Usually benign. Frequent multiform PVCs with R-on-T phenomenon? Now we’re concerned.
Bradycardia and pauses: Sinus pauses >3 seconds, heart block patterns, nocturnal bradycardia. Context matters—athletes frequently show marked nocturnal bradycardia that’s physiologic.
Tachycardia episodes: Sustained vs. non-sustained, SVT vs. VT characteristics, rate and duration, relationship to symptoms.
ST-segment changes: Ischemic shifts require careful analysis and correlation with activity. Artifacts love mimicking ST changes.
Heart rate variability: Reduced HRV associates with autonomic dysfunction and cardiovascular risk, though clinical utility remains debated.
Common Pitfalls and How to Avoid Them
After years of Holter monitoring, I’ve seen these mistakes repeatedly:
1. Inadequate skin prep: Results in poor signal quality, artifacts, and recording failure. Take the extra two minutes to prep properly.
2. Forgetting symptom diaries: Data without clinical correlation is just numbers. Insist patients maintain detailed symptom logs.
3. Over-interpreting artifacts: That “ventricular tachycardia” might be toothbrushing. Review raw tracings, not just automated reports.
4. Ignoring normal variants: Nocturnal bradycardia to 35 bpm in a young athlete isn’t pathologic. Know your normal variants.
5. Single Holter finality: If clinical suspicion remains high despite normal Holter, pursue extended monitoring rather than dismissing symptoms.
The Future: Where Holter Technology Is Heading
We’re witnessing genuine innovation in cardiac monitoring, and it’s exciting:
AI-enhanced analysis: Machine learning algorithms are getting scary good at detecting subtle patterns humans miss. I’m seeing early AFib detection and risk stratification that outperforms traditional analysis.
Implantable loop recorders: For truly rare arrhythmias, injectable monitors providing 2-3 years of continuous recording are game-changers.
Smartphone integration: Consumer-grade ECG apps won’t replace Holters for diagnostic purposes, but they’re useful for preliminary assessment and patient engagement.
Miniaturization: Devices are shrinking to fingernail size without sacrificing functionality.
Real-time alerting: Immediate physician notification of concerning arrhythmias allows faster intervention.
The convergence of wearable technology, AI, and telemedicine is transforming how we approach rhythm monitoring. What seems cutting-edge today will feel primitive five years from now.
Cost Considerations in Sri Lankan Context
Let’s address the elephant in the room: cost matters, especially in resource-limited settings.
Realistic pricing in Sri Lanka:
- Basic 24-hour Holter: LKR 45,000-80,000 ($150-250 USD)
- Premium multi-day wireless: LKR 180,000-300,000 ($600-1000 USD)
- Disposable patches: LKR 60,000-120,000 per use ($200-400 USD)
For practices considering purchasing equipment:
- Initial investment: LKR 300,000-1,200,000 depending on system
- Per-test consumables (electrodes, batteries): LKR 1,500-4,000
- Software licensing: Often bundled, or LKR 150,000-300,000 annually
ROI calculation: With patient charges around LKR 8,000-15,000 per Holter study, and reusable equipment handling 200+ studies annually, break-even typically occurs within 18-24 months.
For smaller practices, rental models or partnering with diagnostic centers may make more financial sense initially.
Setting Up Holter Services in Your Practice
If you’re considering adding Holter monitoring, here’s what you actually need:
Essential requirements:
- Equipment: 2-3 recorder units minimum (one always charging/downloading)
- Quality electrodes: Stock at least 100 electrode sets
- Analysis software: Included with most devices or separate purchase
- Staff training: Minimum 4-8 hours for proper application and troubleshooting
- Space: Dedicated area for patient instruction and device application
- Documentation: Consent forms, instruction sheets, symptom diaries
Workflow considerations:
- Application appointments: 15-20 minutes per patient
- Removal/download: 10 minutes
- Analysis time: 30-60 minutes per study depending on complexity and findings
- Report generation: 15-30 minutes
For a practice seeing 10-15 Holter patients weekly, allocate approximately 10-15 hours of staff time for the complete workflow.
Final Thoughts: Why Holter Monitoring Still Matters
In an era of smartwatches with ECG capabilities and consumer-grade monitoring, you might wonder if traditional Holter monitoring remains relevant. Absolutely yes.
The diagnostic accuracy, continuous recording, and clinical-grade data quality of Holter monitors haven’t been matched by consumer devices. When making treatment decisions about anticoagulation, ablation procedures, or device implantation, you need reliable, comprehensive data—not fragments from a smartwatch.
Holter monitoring represents the sweet spot of cardiac diagnostics: non-invasive, relatively inexpensive, high diagnostic yield, and accessible even in resource-limited settings. It’s not sexy technology, but it’s essential medicine.
For my colleagues in Sri Lanka navigating the challenges of providing quality cardiac care with limited resources, Holter monitoring offers tremendous diagnostic value at reasonable cost. Whether you’re in Colombo, Kandy, or Galle, incorporating Holter services elevates your diagnostic capabilities and improves patient outcomes.
What’s your experience with Holter monitoring in Sri Lankan practice? I’d love to hear about the challenges you’re facing and the solutions you’ve discovered. Drop a comment below, and let’s learn from each other’s experiences.
